Back to Blogs
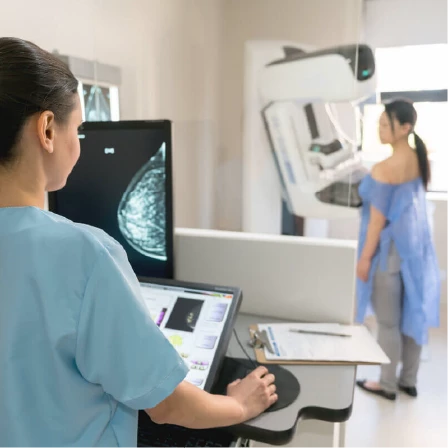
Understanding Breast Cancer Screening Modalities: Mammography, Ultrasound, and MRI
Breast cancer screening is not a single test. It is a set of tools, each designed to answer a different clinical question. Mammography, ultrasound, and MRI all play important roles, but they are not interchangeable. Understanding how they differ helps patients make sense of recommendations and reduces confusion and anxiety.
The goal of screening is to detect breast cancer before symptoms appear, when treatment is often simpler and outcomes are better. Diagnosis, on the other hand, is the process of evaluating a specific concern or abnormal finding. The same imaging tools may be used in both settings, but for different reasons.
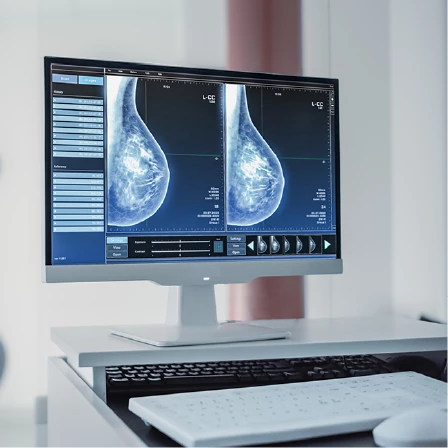
Mammography is the foundation of breast cancer screening.
A mammogram is an X-ray of the breast that can detect very small changes, including calcifications and early masses, long before they can be felt. It is the only screening test proven to reduce breast cancer mortality in the general population.
Mammography works best as a screening tool because it can detect subtle changes that are invisible to the naked eye or to touch. It is particularly good at detecting certain early cancers that may not form a lump.
However, mammography has limitations. Dense breast tissue, which is common and normal, can make interpretation more challenging because both dense tissue and cancers appear white on X-ray. This does not mean mammograms are ineffective, but it may indicate that additional imaging is helpful for certain women.
Ultrasound is a complementary tool.
Breast ultrasound uses sound waves rather than radiation. It is often used to further evaluate a specific area seen on a mammogram or felt on physical exam. Ultrasound is especially helpful in distinguishing solid masses from fluid-filled cysts.
Ultrasound is commonly used in women with dense breasts as an adjunct to mammography and in younger women when mammography may be less informative. It is also useful for guiding biopsies.
Ultrasound is not a replacement for mammography as a screening test. It can miss certain cancers that mammography detects, particularly those that present only as calcifications. Its strength lies in clarification, not replacement.
MRI is a highly sensitive tool used selectively.
Breast MRI uses magnetic fields and contrast material to produce detailed images of breast tissue. It is the most sensitive imaging modality for detecting breast cancer, meaning it can find cancers that other tests may miss.
Because of this sensitivity, MRI is used in specific situations rather than as a routine screening test for everyone. It is often recommended for women at high risk of breast cancer, such as those with known genetic mutations or very strong family histories. It is also used in certain diagnostic scenarios, such as evaluating the extent of known cancer or assessing treatment response.
MRI has limitations as well. Its high sensitivity can lead to false-positive findings, meaning areas that appear concerning but are not cancerous. For this reason, MRI is best used when the benefits clearly outweigh the potential for unnecessary testing.
How these tools work together.
Breast cancer screening and diagnosis are most effective when these modalities are used thoughtfully and in combination rather than in isolation. Mammography provides the baseline. Ultrasound adds clarity. MRI offers depth when risk or complexity is higher.
The choice of imaging depends on age, breast density, personal and family history, genetic risk, symptoms, and prior findings. There is no single “best” test for everyone.
An important distinction is that screening tests are used when a woman feels well and has no symptoms. Diagnostic imaging is used to evaluate a specific concern, such as a lump, pain, or skin change. The same tools may be used, but the intent is different.
Understanding why a particular test is recommended helps patients feel confident rather than alarmed. Being asked to undergo additional imaging does not automatically mean cancer is suspected. Often, it means that the imaging is being thorough.
Breast cancer screening is not about doing more tests. It is about doing the right test, for the right person, at the right time.
When imaging is tailored to the individual, screening becomes not only more effective but also more reassuring.