Back to Blogs

What Follow-Up Care Will I Need After Treatment?
Completing breast cancer treatment is a major milestone. For many patients, it brings relief, pride, and hope. At the same time, it can also bring a new kind of uncertainty. During treatment, you may have seen your medical team frequently. After treatment ends, visits become less frequent, and many patients wonder what comes next.
Follow-up care is not an afterthought. It is an essential part of breast cancer care and long-term health.
The purpose of follow-up care is multifaceted. It allows your medical team to monitor for signs of recurrence, manage lingering or late side effects of treatment, and support your physical and emotional recovery. Just as importantly, it provides reassurance and continuity at a time when many patients feel vulnerable.
The follow-up schedule is individualized. In general, visits are more frequent in the first few years after treatment, when the risk of recurrence is highest. Over time, if everything remains stable, visits become less frequent. The exact timing depends on the type of breast cancer you had, the treatments you received, and your overall health.
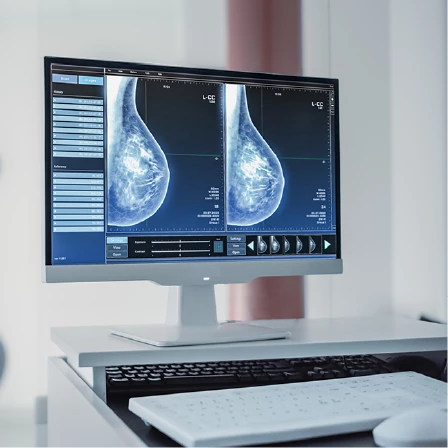
Imaging remains a key component of follow-up. The type and frequency of imaging depend on whether you had breast-conserving surgery or mastectomy, whether reconstruction was performed, and whether any breast tissue remains. These studies are designed to detect changes early, often before symptoms appear.
Follow-up care also addresses side effects that may persist after treatment ends. Some effects improve quickly, while others take longer.
Blood counts, for example, may take several weeks to normalize after chemotherapy. Fatigue is very common and often lingers. Many patients notice gradual improvement over months as strength and stamina return. Gentle, regular physical activity such as walking can play a significant role in recovery.
Hair typically begins to grow back within weeks after chemotherapy ends, though the texture or color may be temporarily altered. Numbness or tingling in the hands and feet, known as neuropathy, may persist for months and gradually improve in most patients, though not always completely.
Changes in taste, appetite, or digestion usually resolve over time, but they can affect nutrition and quality of life in the short term. These issues should be discussed during follow-up visits rather than silently endured.
Cognitive changes, sometimes referred to as “chemo brain,” are also common. Patients may notice difficulty concentrating, forgetfulness, or slower thinking. These changes are real, usually temporary, and tend to improve over several months. Practical strategies, such as focusing on one task at a time and using reminders or calendars, can help during recovery.
Emotional recovery is just as important as physical healing. After treatment, many patients experience fear that the cancer might return. New aches, pains, or symptoms can trigger worry. While these feelings are normal, they should be discussed openly with your healthcare provider. Most post-treatment symptoms are related to healing and adjustment, not recurrence.
Follow-up visits are also a time to focus on overall health. Routine care, including blood pressure checks, cholesterol monitoring, bone health, and preventive screenings, should continue. Breast cancer care works best when coordinated with general medical care.
As time passes and breast cancer–related needs decrease, care may gradually transition from oncology-focused visits to long-term survivorship follow-up and eventually to routine care, with clear guidance on when to return if concerns arise.
Survivorship care is proactive, not passive. It is not about waiting for problems to appear, but about supporting recovery, addressing concerns early, and helping patients regain confidence in their bodies and their lives.
Long-term follow-up should feel structured, supportive, and reassuring. Even after treatment ends, you are not on your own. Care continues, just in a different form.